EPDS and Postpartum Depression: Understanding the Biological Connection
March 10, 2026 | By Clara Maxwell
We often hear the emotional journey of pregnancy and new motherhood described as a "rollercoaster." While the world focuses on the joy of your new arrival, you might be experiencing unexpected feelings of sadness, anxiety, or overwhelm. Friends and family might tell you it is "just your hormones." But what does that actually mean for your brain and body?
Understanding the biological connection between hormonal shifts and mental health is crucial for every new parent. These changes are not just "in your head"—they are physical processes that affect how you think and feel. In this article, we will explore the science behind these transitions. We want to help you identify when a mood shift might be a sign that you need more support.
If you are currently feeling overwhelmed or unsure about your emotions, we invite you to start your screening today. Our free tool helps you understand your symptoms through a scientifically validated lens. Knowing the biological factors at play can empower you to take control of your mental well-being.
The Hormonal Journey of Pregnancy and Postpartum
From the moment of conception, your body begins a massive biological transformation. Hormones act as chemical messengers, telling the body how to grow a new life. However, these messengers also interact with the areas of the brain that regulate mood and stability.
Estrogen and Progesterone: The Dominant Pregnancy Hormones
During pregnancy, levels of estrogen and progesterone increase significantly. By the third trimester, these hormones reach levels that are hundreds of times higher than their usual state. Estrogen helps the uterus grow and maintains the health of the placenta. Progesterone helps keep the uterine muscles relaxed and supports the immune system.
Beyond their physical roles, these hormones have a profound impact on your brain. They influence how you process stress and how you bond with others. When these levels are high, many women feel a sense of "protective" calm. Others may feel more sensitive to emotional triggers. This massive increase sets the stage for the dramatic shift that occurs immediately after birth.
The Sudden Drop: What Happens After Birth
The transition from pregnancy to postpartum involves the most significant hormonal shift a human can experience in such a short timeframe. Within 24 to 48 hours after delivery, estrogen and progesterone levels plummet. They return to their pre-pregnancy levels almost instantly.
This "hormonal crash" is often compared to a sudden chemical withdrawal. Just as the body must adjust to the loss of these hormones, the brain must recalibrate its emotional processing centers. This rapid change is the primary driver of the "baby blues," which affects up to 80% of new mothers. However, for some women, this drop triggers a deeper biological response, leading to what we recognize as hormonal changes postpartum depression.
How Hormones Influence Brain Chemistry and Mood
Hormones don't act alone. They work in complex partnership with the brain's nervous system. When hormone levels shift, they change how brain cells communicate with each other. This is where we see the biology of postpartum depression become clear.
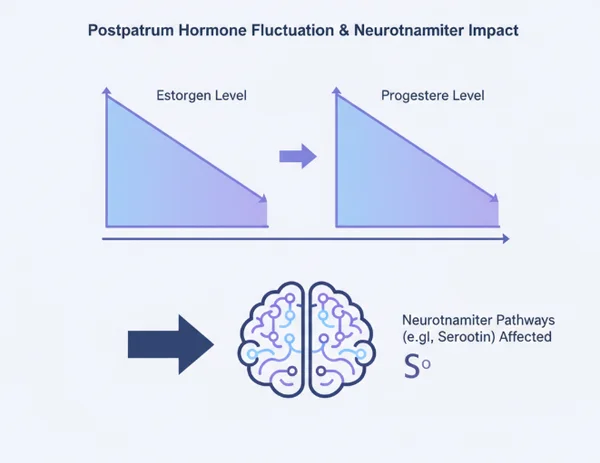
Neurotransmitters and Hormonal Interactions
Neurotransmitters like serotonin and dopamine are responsible for feelings of happiness, motivation, and calm. Estrogen and progesterone play a major role in how these chemicals are produced and used. Specifically, estrogen helps keep serotonin levels stable in the brain.
When estrogen levels drop after birth, serotonin levels can also fall. This can lead to:
- Increased feelings of irritability.
- Disturbed sleep patterns (beyond what the baby causes).
- A loss of interest in activities you once enjoyed.
- Feelings of persistent sadness or hopelessness.
This interaction explains why some women are more sensitive to the perinatal hormone depression link. Their brains may be more vulnerable to the effects of shifting chemical messengers.
The HPA Axis and Stress Response During the Perinatal Period
The Hypothalamic-Pituitary-Adrenal (HPA) axis is the body’s central stress response system. It controls the release of cortisol, the "stress hormone." During pregnancy, the HPA axis changes to protect the developing baby from the mother's stress.
After birth, the HPA axis needs to reset. If this system doesn't return to its normal state, the body remains in high alert. This can manifest as postpartum anxiety or a constant feeling of being "on edge." For many women, the combination of low serotonin and high cortisol creates a perfect storm for mood disorders. If you're wondering if these biological stress markers are affecting your daily life, our free EPDS tool can provide some clarity.
EPDS Assessment Through a Hormonal Lens
The Edinburgh Postnatal Depression Scale (EPDS) is the gold standard for identifying perinatal mood risks. While it is a questionnaire about how you feel, the symptoms it tracks are often rooted in these biological changes.

Why Hormonal Changes Can Trigger EPDS Screening Indicators
Many questions on the EPDS focus on sleep, anxiety, and the ability to feel joy. Because hormones regulate these exact functions, a hormonal imbalance often shows up directly in your EPDS score. For example, if your pregnancy hormones and mood are out of sync, you might find it difficult to laugh or look forward to things with enjoyment.
The screening tool doesn't just look for "sadness." It looks for signs that your brain's regulatory systems are struggling to cope with the postpartum transition. By understanding the EPDS hormonal basis, we can see that a high score is not a sign of personal failure. Instead, it is a signal that your biology needs support.
Distinguishing Normal Hormonal Mood Swings from Clinical Depression
It is normal to feel "weepy" or tired in the first week after birth. This is usually the "baby blues." However, if these feelings last longer than two weeks or become more intense, it may be clinical depression.
Hormonal mood swings typically:
- Peak around day 3 to 5 after birth.
- Fade away within 10 to 14 days.
- Do not prevent you from caring for your baby.
Clinical depression (PPD) is different. It persists and can make daily tasks feel impossible. If you are unsure which one you are experiencing, the best step is to take the test to see where your symptoms fall on the scale.
Managing Hormonal Impacts on Mental Health
While you cannot stop hormones from changing, you can support your body as it navigates these shifts. Management involves both lifestyle adjustments and, when necessary, professional intervention.
Lifestyle Approaches to Support Hormonal Balance
You can help stabilize your internal chemistry through several practical steps. While a new baby makes these difficult, focusing on them can improve your resilience:
- Prioritize Sleep: Lack of sleep spikes cortisol. Even a four-hour block of uninterrupted sleep can help stabilize your mood.
- Nutrition: Foods rich in Omega-3 fatty acids and Vitamin D support brain health and neurotransmitter function.
- Gentle Movement: Short walks can boost endorphins, which are natural mood elevators that counteract the drop in estrogen.
- Social Support: Interaction with supportive friends triggers oxytocin, the "bonding hormone," which naturally lowers stress levels.
When to Consider Professional Support for Hormonal-Related Mood Changes
Sometimes, lifestyle changes are not enough to counter a severe biological shift. If your EPDS score indicates a high risk, it is time to consult a healthcare professional. They may suggest:
- Therapy: Cognitive Behavioral Therapy (CBT) helps the brain create new pathways to manage stress.
- Medication: Some treatments help balance serotonin levels while the body's hormones stabilize.
- Hormone Therapy: In specific cases, doctors may monitor and treat severe hormonal deficiencies.
If you are worried about your mental state, do not wait. You can check your score right now to determine if you should speak with a doctor.
Navigating Your Hormonal Journey
Hormonal fluctuations are a natural part of the perinatal experience. However, when they significantly impact your mental health, understanding these biological factors is the first step toward getting support. These shifts in estrogen, progesterone, and cortisol are powerful. They can change the way you see the world.
By recognizing how hormones contribute to mood changes, you can stop blaming yourself and start looking for solutions. You are not "weak" or a "bad mother." You are a person going through a major biological event. The first step toward feeling like yourself again is awareness.
Take the next step in understanding your perinatal mental health by completing our free EPDS screening today. Our tool provides an instant score and an AI-driven report to help you navigate your journey with clarity and confidence.
The Takeaway
How quickly do hormones change after giving birth?
Hormone levels drop dramatically within 24–48 hours after birth. Specifically, progesterone and estrogen levels decrease to pre-pregnancy levels almost overnight. This rapid change is one of the fastest physiological shifts the human body can undergo. It is a primary cause of the "baby blues."
Can hormonal changes during pregnancy cause depression?
Yes, significant hormonal fluctuations during pregnancy can contribute to depression even before the baby is born. This is known as antenatal depression. While hormones are a major factor, psychological and social stressors also play a role. If you feel consistently low during pregnancy, you should start a screening to assess your risk.
Is the EPDS test affected by hormonal changes?
The EPDS is designed to measure symptoms of depression, regardless of whether the cause is biological, situational, or both. Because hormonal changes cause real physical symptoms—like sleep loss, anxiety, and sadness—the EPDS effectively captures these shifts. It is an excellent tool for identifying when your body's hormonal transition is affecting your mental health.
How long do hormonal mood swings typically last after childbirth?
Most "baby blues" or minor hormonal mood swings resolve within two weeks as your body stabilizes. However, if your mood does not improve after 14 days, it may indicate postpartum depression. For some women, it can take 3 to 6 months for the endocrine system to fully return to its pre-pregnancy state, especially if they are breastfeeding. If you are concerned about how long you have been feeling this way, you can use our tool to get a clearer picture of your status.